Health care spending is growing rapidly in the U.S. and, at 14% of GDP, is much larger than such spending in other industrialized countries. The increase in spending reflects not only changing U.S. demographics but also the use of new, and often costly, treatments, as well as institutional factors relating to health insurance and the structure of the health care industry.
- Heart attacks and treatments
- Productivity and cost changes
- Cross-country evidence
- Conclusions
- References
Health care spending is growing rapidly in the U.S. and, at 14% of GDP, is much larger than such spending in other industrialized countries. The increase in spending reflects not only changing U.S. demographics but also the use of new, and often costly, treatments, as well as institutional factors relating to health insurance and the structure of the health care industry. The question naturally arises, then, whether the increasing cost of treatments has been accompanied by more effective, or, equivalently, more productive, health care services.
This Economic Letter addresses this question by taking a detailed look at treatments for one particular condition, heart attacks. An economic analysis of this disease is important in its own right: in 1999, heart attack patients numbered around 829,000, with medical treatment costing an average of over $20,000 per patient, and heart attacks accounted for around 199,000 deaths. Moreover, because heart attack treatments exhibit the same patterns of growth as the overall health sector, this analysis also can illuminate developments in the entire health sector.
Heart attacks occur when the arteries that supply blood to the heart are blocked. Without oxygen from the blood, part of the heart muscle can die within hours. Heart attack treatments have two goals: in the short run, to limit immediate damage to the heart; in the long run, to reduce arterial blockage.
Heart attack patients typically receive a combination of therapies, which may include both invasive (or surgical) and non-invasive treatments. The primary invasive treatments are heart bypass surgery and angioplasty, both of which are preceded by diagnostic surgical treatments. Bypass surgery involves grafting an artery or vein around the blocked artery. Angioplasty involves using a balloon catheter to break up blockages in arteries. Non-invasive procedures include drug therapies such as clot-busting (thrombolytic) drugs and ACE inhibitors that reduce the pressure of blood flowing to the heart, as well as therapies to change lifestyles, such as exercise and smoking cessation programs.
Several of these procedures highlight the substantial technological progress in treating heart attacks over the past 20 years. For example, many drug therapies, including clot-busting agents, have been developed over this time. Angioplasty was developed in the mid-1980s and further modified in the 1990s to include the use of stents to keep arteries open. In addition, evidence indicates that older procedures, such as bypass surgery, which was introduced in the 1970s, are now more effective.
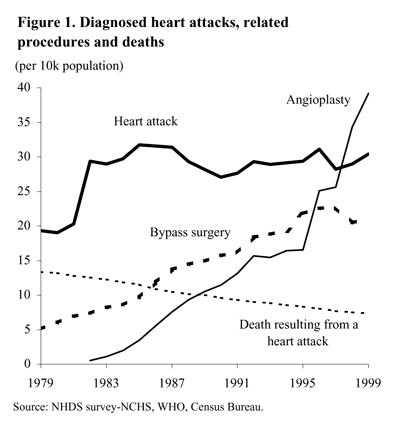
Figure 1 shows the per capita number of heart attacks, deaths from heart attacks, and invasive heart surgeries in the U.S. over the last 20 years. Although the number of heart attacks has been roughly constant, the increase in invasive treatments and the decrease in deaths from heart attacks have been huge. Heart bypass surgery has grown at an average annual rate of 8.4%, and angioplasty has grown from nothing to be even more common than heart attacks. Both treatments also can be used to prevent heart attacks, and this use is growing. Deaths from heart disease are declining at an annual rate of 2.0%.
One can measure the productivity of heart attack treatments by examining their impact on patient health outcomes. Cutler and McClellan (2001) examined a large data set of Medicare patients created from hospital insurance claims to the government and found that, corresponding to the decline in deaths from heart disease, the average life expectancy for elderly heart attack patients has increased by just over one year between 1984 and 1998. Evidence also shows that the quality of life following heart attacks has improved.
The reasons for the increase in the productivity of heart attack treatments are varied and appear to come from new and improved treatments as well as from better use of existing treatments. Heidenreich and McClellan (2001) apportion 34% of the increase in life expectancy after a heart attack between 1975 and 1995 to the increased use of aspirin, a drug that was invented in the 19th century, and a further 17% of the increase to clot-busting drugs. They arrive at these numbers by combining the fact that randomized clinical trials have consistently found a benefit from these treatments with the fact that their usage became much more prevalent between 1975 and 1995. Using Medicare claims data and innovative methods designed to control for the fact that the data were not created from randomized clinical trials, McClellan and Newhouse (1997) find that surgical procedures reduce the probability of a patient’s death within two years by an average of 27%. This suggests that the increased use of surgical procedures contributed to the increased productivity as well.
As medical spending in general has increased in the U.S., so has spending on heart attack treatments. From the claims data, Cutler and McClellan (2001) find that the average Medicare spending per heart attack patient increased by $9,600, from $12,100 in 1984 to $21,700 in 1998, when expressed in constant 1993 dollars. It is not coincidental that both costs and surgical treatments, which are expensive relative to non-invasive treatments, have increased dramatically. By further examining billing data from an unidentified major teaching hospital, Cutler, McClellan, Newhouse, and Remler (1998) show that the real prices of surgical and non-invasive procedures have both remained roughly constant, on average. This implies that the increase in the costs of heart attack treatments is attributable to the increased use of surgical treatments.
Are the increases in the costs of heart attack treatments commensurate with the increased benefits? Answering this kind of question is difficult for many reasons, not least because it involves coming up with a way to place a dollar value on the additional year of life that the treatments provide. Though such measures of the value of life are uncertain and controversial, they generally imply that the value of one year of life is much higher than $9,600, which is the increase in the costs of heart attack treatments between 1984 and 1998 noted above. As a result, research that has studied this issue (see Cutler and McClellan 2001 and Jones 2001) finds that treatments for heart attacks are, on average, more economically supportable today than they were 20 years ago.
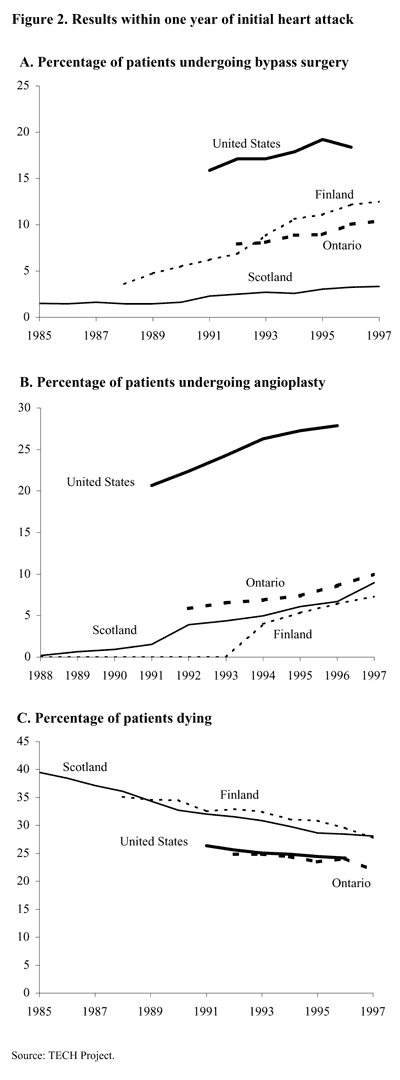
Although there appear to have been significant benefits from the technological change in heart attack treatments, other practice patterns could have been even more effective and cheaper. One can better assess the optimality of treatment patterns by looking at the variation across countries. Figure 2 presents data from four different regions that are representative of cardiac care in the developed world: the U.S., Scotland, Finland, and Ontario, Canada; Panel A shows the percent of patients receiving bypass surgery with one year of a heart attack, Panel B shows the percent of patients receiving angioplasty within one year of a heart attack, and Panel C shows the percent of patients who die within one year of a heart attack. The data are from the Technological Change in Health Care (TECH) project, an international collaboration of investigators from 17 countries, and are based on large, nationally representative samples of patients.
Corresponding to the general trend of health expenditures, the U.S. has much higher rates of bypass and angioplasty than other countries: for instance, in 1997, the one-year bypass and angioplasty rates in the U.S. were 18.4% and 27.9%, respectively, while for Ontario, the rates were 10.4% and 10.0%. But the differences in mortality rates for heart attack patients are much smaller: in 1996, Ontario had a one-year mortality rate of 24.1%, which is very similar to the United States rate of 24.2%; Scotland and Finland had higher mortality rates, but the difference of roughly 5 percentage points between their rates and the U.S. rate was much smaller than the differences in the rates of surgical treatments. Note, however, that we measure only one outcome, patient death. It is possible that the surviving heart attack patients in the U.S. have a higher level of physical function, and hence a higher quality of life, as a result of more invasive surgery.
It might seem that the evidence from the U.S. is at odds with the cross-country evidence. Are new heart attack treatments valuable or not? The apparent contradiction can be resolved by noting that average effects can often be different from incremental effects. In particular, evidence suggests that surgical treatments are valuable on average. However, the incremental surgical treatments done in the United States may not reduce death rates. In other words, angioplasty and bypass surgery reduce the death rates for some patients by a large amount, and yet for many patients they provided little or no benefit.
What economic reasons explain why the United States spends more on heart attack treatments? Chernew, Gowrisankaran, and Fendrick (2002) find that traditional private insurance may provide incentives for hospitals and physicians to open bypass units and hence provide invasive treatments, although managed health care appears to reduce such incentives.
Furthermore, even though the incremental use of invasive surgeries may not help patients, bypass and angioplasty surgery have transformed the prognosis for heart attack patients. The U.S. health care system is different from most other industrialized countries in that services are highly decentralized. Decentralization can lead to vast technological advances but also to unnecessary care. The challenge is to design systems that maximize the diffusion of technological advances while minimizing unnecessary care.
Gautam Gowrisankaran*
Economist
References
Chernew, M., G. Gowrisankaran, and A.M. Fendrick. 2002. “Payer Type and the Returns to Bypass Surgery: Evidence from Hospital Entry Behavior.” Journal of Health Economics 21, pp. 451-474.
Cutler, D.M., and M. McClellan. 2001. “Is Technological Change in Medicine Worth It?” Health Affairs (September/October) pp. 11-29.
Cutler, D.M, M. McClellan, J. Newhouse, and D. Remler. 1998. “Are Medical Prices Declining? Evidence from Heart Attack Treatments.” Quarterly Journal of Economics (November) pp. 991-1024.
Heidenreich, P., and M. McClellan. 2001. “Trends in Treatment and Outcomes for Acute Myocardial Infarction: 1975-1995.” The American Journal of Medicine 110, pp. 165-174.
Jones, C. 2001. “The Economic Return to Health Expenditures.” FRBSF Economic Letter 2001-36 (December 14).
McClellan, M., and J. Newhouse. 1997. “The Marginal Cost-Effectiveness of Medical Technology: A Panel Instrumental-Variables Approach.” Journal of Econometrics 77, pp. 39-64.
*The author thanks the TECH project for providing data. The views expressed herein do not reflect those of the TECH project.
Opinions expressed in FRBSF Economic Letter do not necessarily reflect the views of the management of the Federal Reserve Bank of San Francisco or of the Board of Governors of the Federal Reserve System. This publication is edited by Anita Todd and Karen Barnes. Permission to reprint portions of articles or whole articles must be obtained in writing. Please send editorial comments and requests for reprint permission to research.library@sf.frb.org