It’s been almost a decade since the Federal Reserve Bank of San Francisco launched the Healthy Communities Initiative in partnership with the Robert Wood Johnson Foundation, and the community development field has made significant progress in that time—both in terms of widespread recognition of the impact that social determinants have on health, as well as innovative partnerships that bridge health and community development. These efforts have tended to focus on the connections between place and physical health, such as neighborhood revitalization as a strategy to improve the health of low-income communities, with a focus on reducing rates of preventable chronic disease like asthma, diabetes, and obesity. However, our efforts have been less explicit about mental, emotional, and behavioral health, which are equally important in overall health promotion. As the World Health Organization (WHO) says, “There is no health without mental health.”1 This presents an opportunity for the community development field to advance the healthy communities conversation by explicitly recognizing the relationship between mental health and physical health, and the role that social factors play in both aspects of overall wellbeing.
“Upstream” social factors, such as neighborhood conditions or household financial well-being, are important determinants of mental health and can influence factors such as emotional resilience, social connectedness, and self-efficacy. The pursuit of improved population health should include upstream strategies that address community conditions and their underlying structural drivers as a means of promoting good mental health. This article provides a brief introduction to the relationship between community development and mental health. The connections are complex and multifaceted, and warrant further exploration and partnership across both fields.
Understanding Mental Health
According to the WHO, “mental health is defined as a state of well-being in which every individual realizes his or her own potential, can cope with the normal stresses of life, can work productively and fruitfully, and is able to make a contribution to her or his community.”2 Notably, mental health is not simply the absence of mental illness. This is an important distinction as the terms “mental health” and “mental illness” are often used interchangeably, when in fact they describe different dimensions. Every person experiences ups and downs in their mental health, but not every person will experience symptoms of mental illness. The onset, duration and intensity of symptoms is dependent upon multiple factors, including a person’s internal resilience and their access to resources that provide stability and comfort.
An estimated 1 in 5 adults lives with a mental illness (44.7 million people in 2016).3 The financial cost, which includes mental health care expenditures as well as lost earnings and public disability insurance, was estimated to be at least $267 billion in the U.S. in 2012.4 The World Economic Forum estimates that the global costs for mental disorders are greater than the costs of diabetes, respiratory disorders, and cancer combined.5 In addition, the medical costs for treating patients who have concurrent chronic medical and mental health/substance use disorder conditions are two to three times higher compared to the costs for patients who don’t have “comorbid” mental health conditions (the projected additional healthcare costs were estimated to be $406 billion in 2017).6 Substance abuse disorders are a related, but distinct, category from mental disorders, and the two are often grouped under the broader umbrella term of behavioral health disorders. Substance abuse and mental health challenges often overlap; of the estimated 20.2 million American adults who had a substance use disorder in 2014, roughly 40 percent had a co-occurring mental illness.
Mental health is influenced by a variety of individual attributes, environmental factors, and social and economic circumstances. As a result, people differ in their emotional resilience and “hardiness” which means that individuals experience symptoms of mental distress at varying levels in the face of stress and trauma. There are a number of risk factors that negatively impact mental health at both the individual and community levels, which have important implications across the life course (Fig. 1).7
Figure 1
Overview of Risks to Mental Health over the Life Course
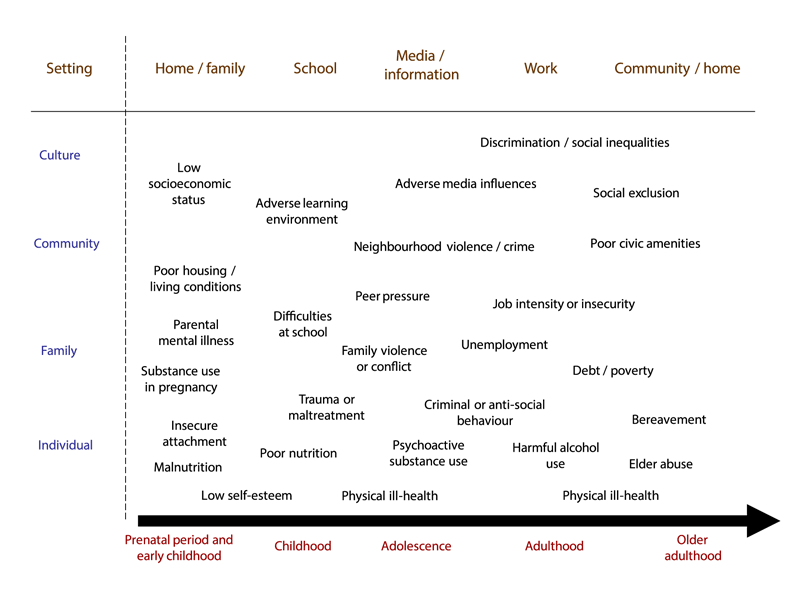
Community development has the power to influence health at the population level by supporting the physical, social, and civic infrastructure that makes health possible. Achieving population-level mental health, consistent with the WHO definition, is a necessary component of achieving broader population health, and it requires approaches that go beyond a focus on individual-level clinical treatment for those struggling with mental health challenges. We have the opportunity to recognize the ways in which community-level factors influence mental health, which elevates the need for strategies that focus on prevention.
Poverty is a Driver of Poor Mental Health
Poverty itself is a major risk factor for poor mental health. Research shows that community development-related issues such as unstable housing and unemployment are connected in a complex negative cycle with poor mental health (Fig. 2).9 There is a growing awareness of the need to explicitly address the mental health needs of low-income populations, recognizing that they are more likely to face negative risk factors such as adverse childhood experiences, social isolation and loneliness, discrimination, and detachment from academic or work achievement. These negative experiences can diminish a person’s sense of control, self-efficacy, connectedness, and hope, all of which are important elements for resilience and mental health promotion. People in poverty are also less likely to have protective factors that promote mental health, including many of the things that community development works to provide, such as stable housing, supportive community networks, and financial security. Low-income children and adults also face barriers to access to mental health services, including cost, lack of insurance, inflexible clinic hours that do not accommodate people in low-wage jobs, and long distances to services, particularly for rural patients.10 In addition, the stigma of mental illness, combined with the stigma of poverty, can also act as a barrier to accessing mental health care.
Figure 2
Positive and Negative Factors that Influence Mental Health
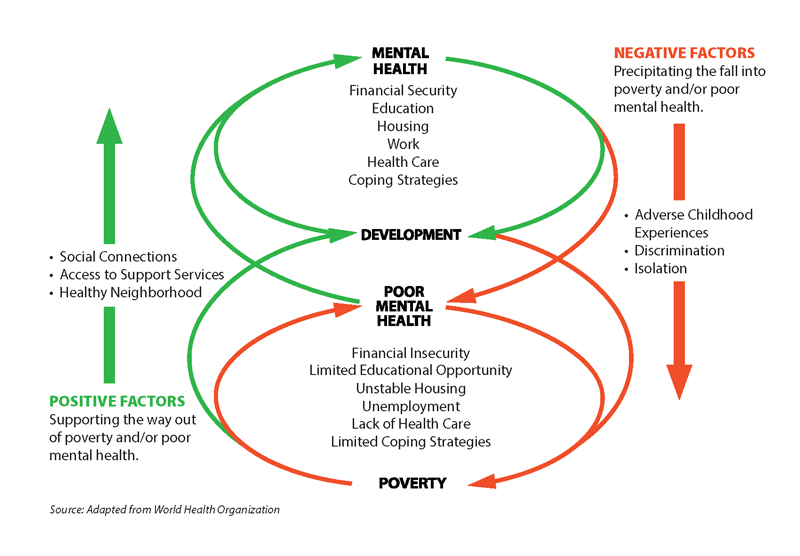
Although researchers are still debating the causal pathways between poverty and poor mental health, it is clear that the two are closely linked. For example, data from the Center for Disease Control’s National Health Interview Survey reveal that having less income increases the likelihood of having “serious psychological distress,” defined as being severe enough to cause moderate-to-serious impairment in social, occupational, or school functioning and to require treatment (Fig. 3).11 People below the federal poverty line were more than seven times more likely to have severe psychological distress than their well-to-do peers.
Figure 3
Percentage of adults with serious psychological distress, by income and by race and ethnicity: United States, 2009-2013
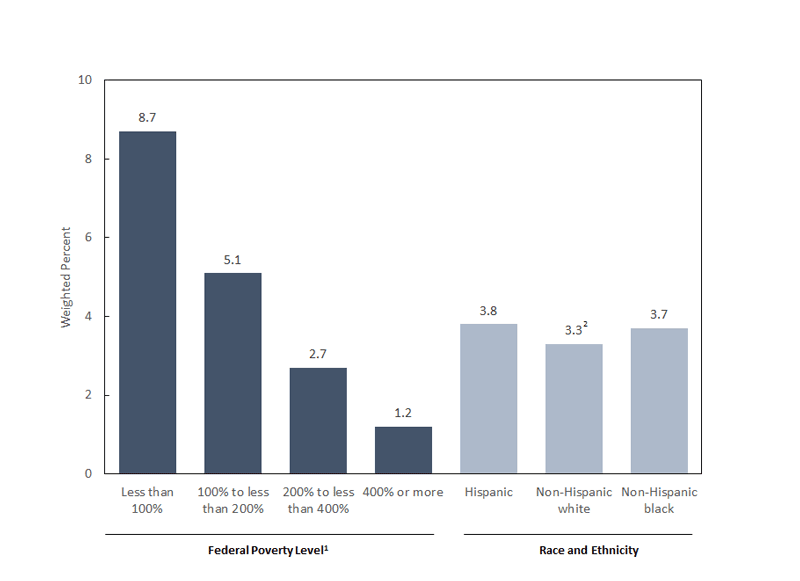
Notes: (1) Significant decreasing linear trend by poverty level; (2) Significantly lower than for other races and ethnicities.
Mental Health is Essential to Achieving Equity
The data also reveal that demographic dimensions such as gender and race play a role. Serious psychological distress affects 3.3 percent of non-Hispanic white adults, which is significantly lower than the rate for non-Hispanic blacks and Hispanics, at 3.7 percent and 3.8 percent respectively (Fig. 3). In addition, in every age group, women were more likely to have serious psychological distress than men (Fig. 4). Considering the intersection of race, gender, and income, and the negative impacts of structural discrimination, the data suggest that low-income people of color, and in particular low-income women of color, may need particular attention when it comes to mental health promotion.
Figure 4
Percentage of adults with serious psychological distress, by sex and age: United States, 2009-2013
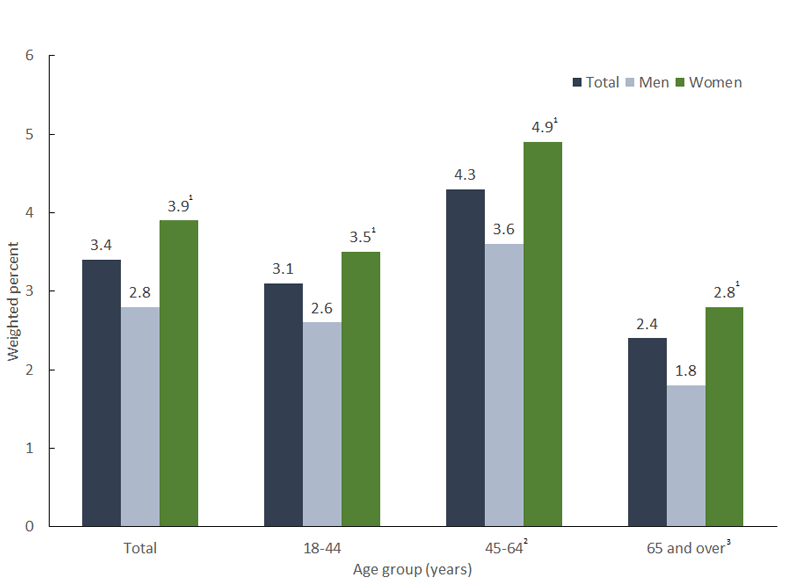
Notes: (1) Significantly higher percentage of women with serious psychological distress than men; (2) Significantly higher percentage with serious psychological distress than other age groups; (3) Significantly lower percentage with serious psychological distress than other age groups.
Mental Health Matters for Community Development
Mental health promotion across the life course is critical for supporting the economic resilience and mobility of low-income people, a key aim of community development efforts. For example, there is clear evidence that poor mental health is associated with reductions in labor force participation and employment.12 It is also both a consequence of and risk factor for unemployment.13 Mental health problems among children have a severe negative impact on educational outcomes, which can limit future economic wellbeing. Approximately 50 percent of students age 14 and older who are living with a mental illness drop out of high school, which is the highest dropout rate of any disability group.14 Among children ages 6-17 years old who were defined as needing mental health services, nearly 80 percent did not receive mental health care.15 Perhaps most critically, adverse childhood experiences, which include abuse, neglect, having an incarcerated household member, or substance misuse within the household, are risk factors for poor mental health and have been linked to a number of negative health and well-being outcomes, including risky health behaviors, chronic health conditions, and early death.16
The broader issue of behavioral health, which includes substance use disorders, also has major implications for communities and the economy. Federal Reserve Chairman Jerome Powell discussed the opioid crisis during a recent appearance before a Senate committee, stating “It’s having a terrible human toll on our communities and also it matters a lot for the labor force participation rate and economic activity in our country.”17 A recent study by the Trust for America’s Health and Well Being Trust reports that in 2016, the most recent year of data available, 142,000 Americans died from alcohol- and drug-induced fatalities and suicide, the highest number ever recorded.18 The economists Angus Deaton and Anne Case have suggested that the dramatic rise of these “deaths of despair,” which are increasing in all parts of the country and at every level of urbanization, are accompanied by a measurable deterioration in economic and social wellbeing, which has become more pronounced for each successive birth cohort.19
Cross-Sector Partnerships as a Way Forward
In his recent book Lost Connections, journalist Johan Hari synthesizes decades of social and behavioral science and medical research and finds that poor mental health is driven by a range of factors outside of individual genetic and biochemical factors, which include:20
- Disconnection from meaningful work
- Disconnection from other people
- Disconnection from childhood trauma
- Disconnection from status and respect
- Disconnection from the natural world
- Disconnection from a hopeful or secure future
Reflecting on these drivers of poor mental health, it becomes clear that the community development field has a meaningful role to play in addressing these root causes. The community development and mental health fields have a critical opportunity to work together and leverage each other’s strengths to support the mental health of low-income communities. This can include:
- Expanding trauma-informed practices, including critical interventions for young children
- Considering mental health promotion in community design, which includes community gathering spaces and natural elements
- Interventions that increase social connections and foster a sense of belonging
- Community violence prevention efforts
- Partnering to offer community-based mental health and behavioral health services
- Developing community-driven mental health campaigns and arts and cultural strategies to reduce stigma and shame
- Raising awareness of mental health issues among front line staff and providing resources such as training on mental health first aid
As social innovator Liz Ogbu says, “When we work in low-income communities, we tend to focus on need because the lack of resources is so readily apparent and visible. We don’t focus enough on aspiration. In fact, having an aspiration is a luxury we rarely ascribe to poor people, but they’re human; they have hopes and dreams.”21 Ultimately, this work is about ensuring that every community can be a place of healing and connectedness, where aspiration is a given, and building hope for the future is as central to our field as building housing.
1. “Mental health: strengthening our response,” World Health Organization, March 30, 2018.
2. “Mental health: a state of well-being,” World Health Organization, August 2014.
3. “Mental Illness” National Institute of Mental Health, November 2017.
4. Thomas Insel, “Mental Health Awareness Month: By the Numbers,” National Institute of Mental Health, May 15, 2015.
5. D.E. Bloom, et al. “The Global Economic Burden of Noncommunicable Diseases,” World Economic Forum, 2011.
6. Stephen Melek, et al., “Potential economic impact of integrated medical-behavioral healthcare,” Milliman, January 2018.
7.Center for Behavioral Health Statistics and Quality, “Behavioral health trends in the United States:
Results from the 2014 National Survey on Drug Use and Health” (HHS Publication No. SMA 15-4927, NSDUH
Series H-50).
8. Ibid.
9. “Breaking the Vicious Cycle between Mental Ill-Health and Poverty,” World Health Organization, Mental Health Core to Development Information Sheet, Sheet 1, 2007.
10. Stacy Hodgkinson, et al., “Improving Mental Health Access for Low-Income Children and Families in the Primary Care Setting,” Pediatrics 139, no. 1.
11. Judith Weissman, et al. “Serious Psychological Distress among Adults: United States, 2009-2013,” National Center for Health Statistics Data Brief, No. 23, May 2015.
12. Pinka Chatterji, Margarita Alegria, and David Takeuchi, “Psychiatric Disorders and Labor Market Outcomes: Evidence from the National Comorbidity Survey-Replication,” Journal of Health Economics 30, no. 5 (2011): 858–868.
13. Sarah Olesen, et al., “Mental health affects future employment as job loss affects mental health: findings from a longitudinal population study,” BMC Psychiatry 13, no. 144 (2013).
14. U.S. Department of Education, Twenty-third annual report to Congress on the implementation of the Individuals with Disabilities Education Act, Washington, D.C., 2001.
15. S. Kataoka, L. Zhang, and K. Wells, “Unmet need for mental health care among U.S. children: variation by ethnicity and insurance status,” American Journal of Psychiatry 159, no. 9 (2002): 1548-55.
16. “Adverse Childhood Experiences” Centers for Disease Control and Prevention, April 1, 2016
17. Jeff Cox, “Opioid addition is keeping a high percentage of people out of the workforce, Fed chairman says,” CNBC, July 17, 2018
18. “Pain in the Nation Update: Deaths from Alcohol, drugs, and suicide reach the highest level ever recorded,” Trust for America’s Health and Well Being Trust, February 2018.
19. Anne Case and Sir Angus Deaton, “Mortality and morbidity in the 21st century,” Brookings Papers on Economic Activity
20. Johann Hari, Lost Connections: Uncovering the Real Causes of Depression–and the Unexpected Solutions (New York: Bloomsbury, 2018).
21. “Design, Culture, and Complex Problems: Q&A with Liz Ogbu,” SPARCC
